Torticollis, also known as wryneck or Loxia, is a condition characterized by anomalous, uneven posture of neck or head. This is one of the wide spectrum of disorders that indicates flexion, twisting or extension of muscles of neck beyond its range of motion. The disorder causes twisting of neck on one side which in turn causes the head to tilt. The word ‘Torticollis’ is derived from Latin terms ‘tortus’ for ‘twisted’ and ‘collum’ for ‘neck’. The condition can be hereditary wherein it may develop gradually or from a trauma. It may also be an outcome of medicinal side-effects.
Causes of Torticollis and Classification
There are several factors recorded that can cause torticollis. These factors may include fibrosis, congenital anomalies of spine, toxic influence on brain or traumatic brain injuries. Here are two common classifications along with causes.
Congenital Torticollis
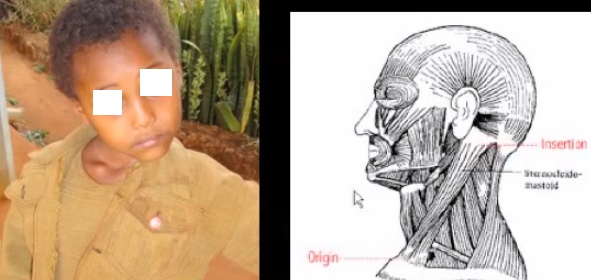
Congenital Torticollis or Congenital Muscular Torticollis is a condition that is present from birth. Etiology of this kind of anomaly is not certainly known. Intrauterine faulty positioning or even birth trauma is considered as the most common cause of congenital wryneck. Such circumstances would lead to sternocleidomastoid muscle of neck. This causes intense contraction or shortening of this muscle restricting the range of motion. Lateral bending and rotational movement becomes significantly affected. Under this condition the head is often tilted on the side of the neck with muscle contraction.
Approximately 2% of the population is affected with ‘congenital torticollis’. In some cases sternocleidomastoid tumor is also noticed in contracted muscle goupr, usually by the age of two to four weeks. Though this tumor may disappear by the age of 8 months the fibrotic muscles remains persistent. The condition is initially treated using physical therapies such as stretching that releases tightness, strengthening exercises for muscular balance, etc. In some cases TOT collar is suggested. In around 5 to 10 percent of all cases surgery may be needed as the condition does not respond to stretching and exercises.
Acquired Torticollis
Non-congenital Torticollis or Acquired Torticollis can be caused due to scarring or cervical vertebrae associated diseases. Adentitis, rheumatism, protruded cervical glands, cerebellar tumor etc are some of the conditions that can lead to acquired wryneck. The condition can be spasmodic (abnormal neuromuscular activity) or permanent. The latter may occur due to tuberculosis of spine which is referred to as Pott’s Disease. Spontaneously occurring self-restricting type of wryneck is more common than other. In such a case one or more neck muscles are affected. Usually the associated muscle in this condition is the trapezius muscle. Posterior fossa tumor, commonly, tumor of base of skull, may compress the vital nerves of the neck muscles leading to Loxia. To treat such a condition surgical intervention is often needed.
Nerves can become irritated due to posterior pharynx infection. This can serve to be a cause of wryneck. If these infections are not severe then they can be treated using antibiotic; however, in extreme cases surgery may be suggested. Infection and debridement of adenoids can lead to Grisel’s syndrome which is partial displacement of upper cervical joints. This occurs due to laxity of inflamed ligaments resulted due to infection. Surgical intervention or other manipulations of neck may help in dealing with the condition. Acquired torticollis may also sometimes result out of antipsychotic drug usage.
Symptoms of Torticollis
Spasmodic torticollis is anomalous contraction of the muscle in one side of the neck. This causes sideward tilt of the head. Muscles in the neck and between shoulder and neck are often tender and tense. Affected people often avoid tilting the head on the other side. Some other common symptoms of the condition include:
- Head pain
- Pain in the back
- Shoulder pain
- Cramps at neck
- Tightness of muscles
- Burning sensation
Diagnosis of Torticollis
Diagnosis of Torticollis in child starts with interrogation on history to understand the circumstances of birth and chances of injury. Physical evaluation helps in determining the restriction on ability to bend and rotate neck towards the opposite side from the one that is affected. Hypothetically congenital torticollis mostly affects the right side. Diagnosis of the condition should include complete neurological examination. Possibilities of related conditions such as clubfoot or dysplasia of the hip should be ruled out. X-ray or Gama ray evaluation should be done on cervical spine to determine any anomalies associated with the bones. In case structural issue is suspected then MRI should be suggested to the patient.
Torticollis treatment
Treatment for torticollis is mostly focused on relieving contraction of the affected neck muscle. Usually treatment regimen includes combination of medicines, physical aid, physical therapy, exercises, botulinum toxins and sometimes surgery. In some cases the condition may resolve within days or may take weeks. Only a few cases may persist for months or years. Consistent neck muscles spams should be diagnosed by a surgeon or neurologist.
Physiotherapist may help you get relieve by suggesting exercises both for children and adults. He may suggest you exercises which should be done at least 5 times during the day. The focus of exercises will remain on strengthening neck and improve motor actions. The condition is more difficult to be treated in adults as compared to children. In case of adults one can apply heat pad for around 10 minutes before starting exercises. This will enhance supply of blood to affected region and help while doing exercise. It is essential that these exercises are done in appropriate manner; hence, seek professional assistance before you learn doing it on your own.
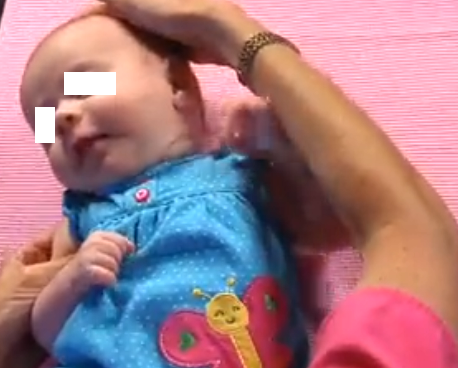
Torticollis Exercises for the Baby
One of the exercises is to hold the baby’s ear and bring the side of the head towards the shoulder. Keep it this way for ten seconds and do this 3 times. Now follow suit for the other side. The other exercise is holding the chin of the baby and bringing it to the shoulder. Hold it this way for ten seconds and do this exercise three times. Do the same for the other side. You may do this exercise 6 times a day during the course of diaper rash for six to eight weeks and see if there is any change. If there is no positive change, you may seek the help of a professional physiotherapist.
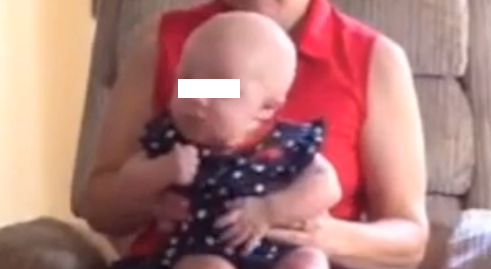
Torticollis Pictures